einstein (São Paulo). 01/Apr/2011;9(2 Pt 1):140-4.
Allogeneic hematopoietic stem cell transplantation in children with primary immunodeficiencies: Hospital Israelita Albert Einstein experience
DOI: 10.1590/S1679-45082011AO2007
ABSTRACT
Objective:
To report the experience of a tertiary care hospital with allogeneic hematopoietic stem cell transplantation in children with primary immunodeficiencies.
Methods:
Seven pediatric patients with primary immunodeficiencies (severe combined immunodeficiency: n = 2; combined immunodeficiency: n = 1; chronic granulomatous disease: n = 1; hyper-IgM syndrome: n = 2; and IPEX syndrome: n = 1) who underwent eight hematopoietic stem cell transplants in a single center, from 2007 to 2010, were studied.
Results:
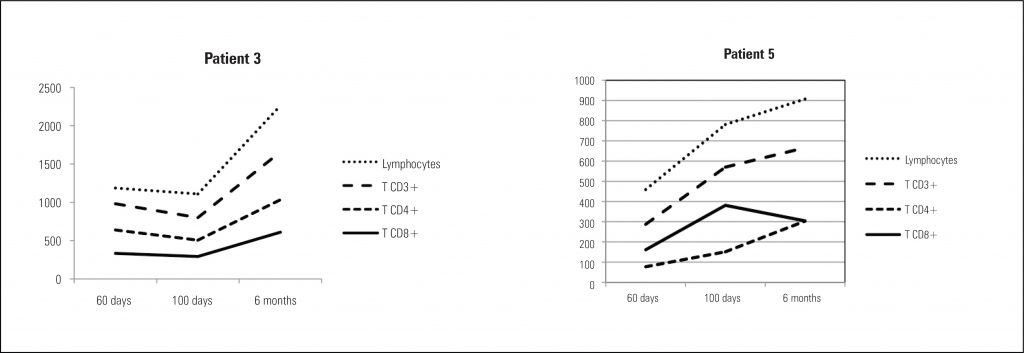
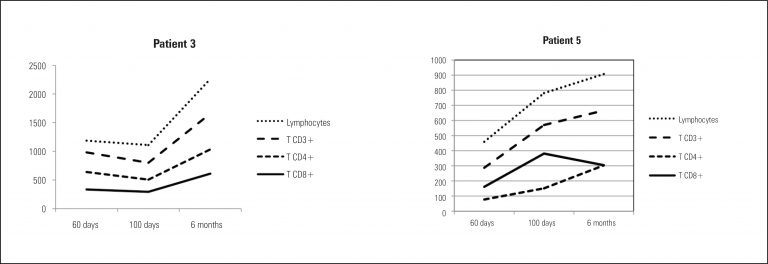
Two patients received transplants from HLA-identical siblings; the other six transplants were done with unrelated donors (bone marrow: n = 1; cord blood: n = 5). All patients had pre-existing infections before hematopoietic stem cell transplants. One patient received only anti-thymocyte globulin prior to transplant, three transplants were done with reduced intensity conditioning regimens and four transplants were done after myeloablative therapy. Two patients were not evaluated for engraftment due to early death. Three patients engrafted, two had primary graft failure and one received a second transplant with posterior engraftment. Two patients died of regimen related toxicity (hepatic sinusoidal obstruction syndrome); one patient died of progressive respiratory failure due to Parainfluenza infection present prior to transplant. Four patients are alive and well from 60 days to 14 months after transplant.
Conclusion:
Patients’ status prior to transplant is the most important risk factor on the outcome of hematopoietic stem cell transplants in the treatment of these diseases. Early diagnosis and the possibility of a faster referral of these patients for treatment in reference centers may substantially improve their survival and quality of life.
783