einstein (São Paulo). 30/May/2019;17(3):eAO4467.
Laryngotracheal separation in pediatric patients: 13-year experience in a reference service
DOI: 10.31744/einstein_journal/2019AO4467
ABSTRACT
Objective:
To evaluate clinical stability of neurologically impaired children and adolescents with recurrent pneumonia submitted to laryngotracheal separation.
Methods:
Between October 2002 and June 2015, 92 neurologically impaired children from a reference service, with median age of 68.5 months were submitted to laryngotracheal separation. Data were evaluated and statistical analysis was made by Student’s t test and Pearson’s χ2 test (significance level adopted of 95%).
Results:
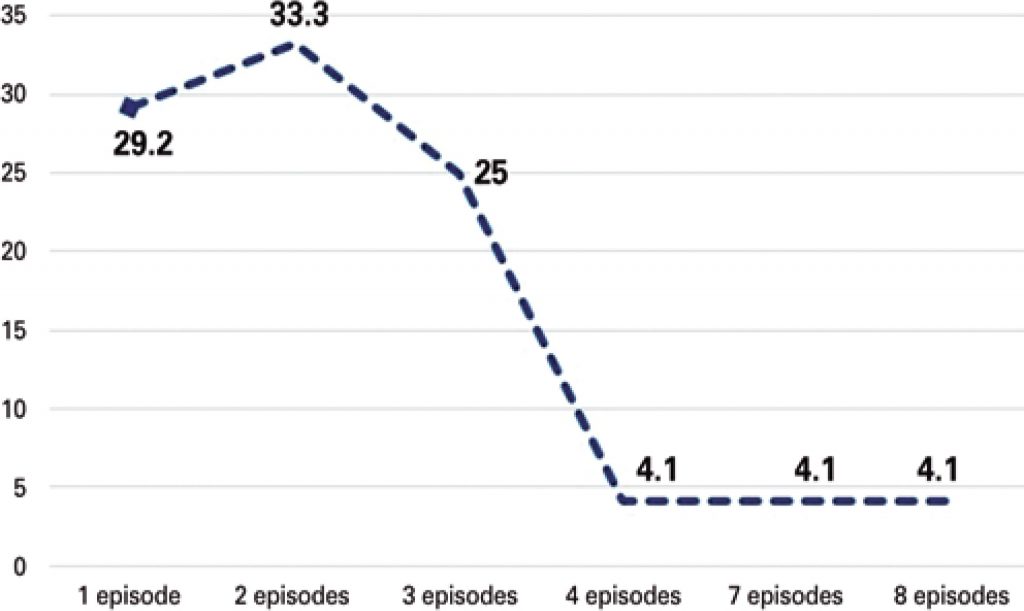
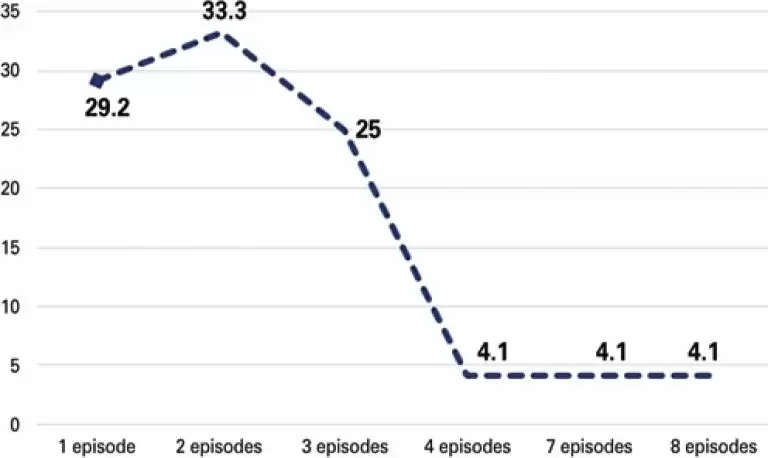
Fifty-three children were male (57.6%). Forty-six children required admission to intensive care, and 42.4% needed mechanical ventilation. We observed that 90.2% of patients were exclusively fed by gastrostomy and 72.4% of the gastrostomies were performed before the tracheal surgery. Thirteen (14.1%) children had postoperative complications as follows: fistulae (5.4%), bleeding (4.3%), granuloma (2.2%) and stenosis (3.2%). A total of 24 patients had pneumonia in the postoperative period (26.1%), but there was a significant drop in occurrence of this condition after surgery (100% versus 26.1%; p<0.001). Twenty-three patients (25%) died. Postoperative complications were similar when comparing patients who died and those that presented good outcome (16.7% versus 13.2%; p=0.73).
Conclusion:
When well-indicated, the laryngotracheal separation reduces the incidence of postoperative pulmonary infections, thus improving quality of life and reducing admissions to hospital. Laryngotracheal separation should be indicated as a primary procedure in patients with cerebral palsy and recurrent aspiration pneumonia.
Keywords: Larynx/surgery; Trachea/surgery; Pneumonia; aspiration; Nervous system diseases; Child
1,497